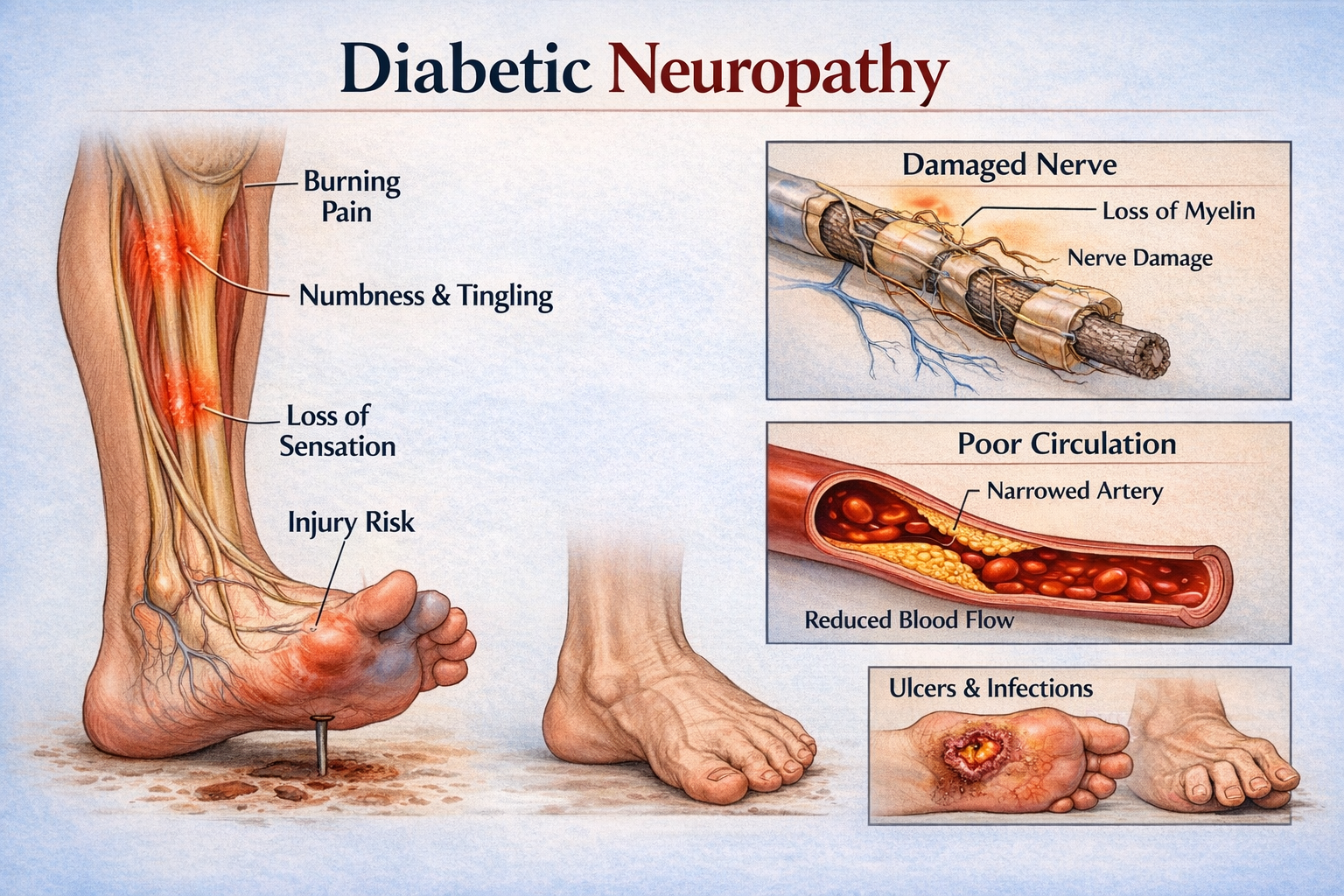
Diabetic nerve pain, also known as diabetic neuropathy, affects millions of people worldwide. For many individuals living with diabetes, symptoms such as burning, tingling, numbness, and sharp pain in the feet or hands can gradually become part of daily life.
While high blood sugar levels are often blamed as the primary cause of diabetic neuropathy, another critical factor frequently goes overlooked: circulation.
Healthy blood flow plays a crucial role in keeping nerves nourished, oxygenated, and functioning properly. When circulation becomes impaired—something that commonly occurs in diabetes—the nerves begin to suffer. Over time, reduced blood flow can damage nerve fibers and worsen pain, numbness, and loss of sensation.
Understanding the connection between circulation and diabetic nerve pain can help individuals living with diabetes take proactive steps to slow nerve damage, relieve symptoms, and improve long-term health.
Understanding Diabetic Neuropathy
Diabetic neuropathy refers to nerve damage caused by prolonged elevated blood glucose levels. Over time, high glucose levels can injure nerves throughout the body, but the most common type is peripheral neuropathy, which affects the feet and legs first.
Common symptoms include:
Burning sensations in the feet
Tingling or “pins and needles”
Numbness or reduced ability to feel pain
Sharp or stabbing pain
Increased sensitivity to touch
Muscle weakness
Balance problems
Many people assume neuropathy happens suddenly. In reality, the condition typically develops slowly over years, often beginning with subtle changes in circulation.
Why Circulation Is Essential for Nerve Health
Nerves are metabolically active tissues that require a constant supply of oxygen, nutrients, and energy to function properly. These vital elements are delivered through the bloodstream.
Healthy circulation provides nerves with:
Oxygen for cellular metabolism
Glucose for energy production
Essential vitamins and minerals
Anti-inflammatory immune support
Removal of metabolic waste products
When blood flow becomes restricted, nerves begin to experience metabolic stress. Over time, this stress can lead to inflammation, degeneration, and impaired nerve signaling.
This is one of the key reasons circulation problems can worsen diabetic nerve pain.
How Diabetes Impairs Circulation
Diabetes affects the body in multiple ways that can compromise blood flow. Several physiological changes contribute to circulation problems.
Damage to Blood Vessels
Chronic high blood glucose levels damage the lining of blood vessels, a condition known as endothelial dysfunction. This damage causes vessels to become stiff, narrowed, and less able to deliver adequate blood flow to tissues.
Small blood vessels that supply nerves—called vasa nervorum—are particularly vulnerable.
When these tiny vessels become damaged, the nerves they support begin to deteriorate.
Increased Inflammation
Diabetes promotes systemic inflammation, which can further damage blood vessels and reduce circulation.
Inflammation causes swelling inside vessel walls, narrowing the passage where blood flows. This restricts oxygen delivery to nerve tissue.
Over time, chronic inflammation contributes to the progression of neuropathy.
Reduced Nitric Oxide Production
Nitric oxide is a molecule that helps blood vessels relax and widen. In people with diabetes, nitric oxide production often becomes impaired.
Without sufficient nitric oxide, blood vessels remain constricted, reducing circulation to extremities such as the feet and hands.
Poor vasodilation contributes significantly to neuropathic pain.
Thickened Blood and Reduced Microcirculation
High glucose levels can also make blood thicker and more sluggish, which interferes with microcirculation.
The smallest blood vessels, called capillaries, are responsible for delivering nutrients to nerves. When these vessels become compromised, nerve tissue may experience oxygen deprivation.
This process contributes to nerve damage and pain.
The Link Between Poor Circulation and Nerve Pain
Reduced circulation does not simply damage nerves—it also contributes directly to the pain experienced in diabetic neuropathy.
Several mechanisms explain this relationship.
Oxygen Deprivation
When nerves do not receive enough oxygen, they become dysfunctional. This condition, known as ischemia, can trigger pain signals within nerve fibers.
Ischemic nerves may fire erratically, producing sensations such as burning or electric shocks.
Accumulation of Metabolic Waste
Healthy circulation helps remove waste products from tissues. When circulation is impaired, these metabolic byproducts accumulate around nerve fibers.
Waste buildup irritates nerves and contributes to inflammation, which increases pain sensitivity.
Increased Nerve Sensitivity
Damaged nerves often become hypersensitive, amplifying pain signals even in response to mild stimuli.
This is why some people with diabetic neuropathy experience discomfort simply from the touch of clothing or bed sheets.
Poor circulation exacerbates this hypersensitivity.
Why the Feet Are Most Affected
Diabetic neuropathy usually begins in the feet and lower legs because these areas are the farthest from the heart.
Blood must travel a longer distance to reach these extremities. When circulation becomes compromised, the feet often receive the least oxygen and nutrients.
Additional factors that worsen circulation in the feet include:
Gravity slowing blood return
Reduced physical activity
Damage to small vessels
Compression from tight footwear
Over time, poor circulation in the feet can lead to severe complications, including ulcers, infections, and in extreme cases, amputation.
Early Warning Signs of Circulation Problems in Diabetes
Recognizing circulation issues early can help prevent severe nerve damage.
Common signs of reduced circulation include:
Cold feet or hands
Numbness or tingling
Slow wound healing
Skin discoloration
Hair loss on legs
Shiny or thin skin
Cramping in the legs while walking
If these symptoms appear alongside nerve pain, circulation may be playing a significant role in the progression of neuropathy.
Strategies to Improve Circulation and Reduce Diabetic Nerve Pain
Although diabetic neuropathy can be challenging, improving circulation can significantly help slow nerve damage and relieve symptoms.
Several strategies support better blood flow.
Optimize Blood Glucose Control
Maintaining stable blood glucose level is the most important step in protecting circulation.
When blood glucose level remains elevated, vascular damage continues to worsen.
Strategies to support healthy glucose levels include:
Balanced nutrition
Regular physical activity
Stress management
Adequate sleep
Medical supervision
Improved metabolic health protects both nerves and blood vessels.
Increase Physical Activity
Movement is one of the most effective ways to improve circulation.
Exercise helps:
Stimulate blood flow
Improve vascular flexibility
Enhance insulin sensitivity
Deliver oxygen to nerve tissue
Low-impact exercises such as walking, swimming, cycling, and stretching can be particularly beneficial for people with neuropathy.
Even brief movement throughout the day can improve circulation.
Support Lymphatic Flow
The lymphatic system works alongside circulation to remove toxins, excess fluid, and inflammatory compounds from tissues.
When lymphatic flow becomes sluggish, swelling and inflammation may worsen nerve irritation.
Therapies such as lymphatic drainage therapy can help support circulation, reduce fluid buildup, and promote tissue healing.
Improved lymphatic movement also helps enhance microcirculation around nerves.
Nutritional Support for Nerve and Vascular Health
Certain nutrients support circulation and nerve repair.
These include:
B vitamins, especially B12 and B1
Alpha-lipoic acid
Magnesium
Omega-3 fatty acids
Antioxidants such as vitamin C and E
Because individual responses to supplements therapy varies, it is important to have comprehensive nutrition tests and consultation for precision intervention. A nutrient-dense diet rich in vegetables, healthy fats, lean proteins, and fiber also supports vascular health and reduces inflammation.
Stress Reduction and Nervous System Balance
Chronic stress activates the sympathetic nervous system, which constricts blood vessels and reduces circulation to extremities.
Stress management techniques such as neurofeedback, biofeedback, neuromeditation, breathwork, massage therapy, and relaxation practices can help restore vascular balance.
Improving nervous system regulation can support better blood flow throughout the body.
Therapeutic Bodywork and Circulation Support
Manual therapies that stimulate circulation can provide relief for individuals with diabetic nerve pain.
These therapies include:
Therapeutic massage
Lymphatic drainage
Myofascial therapy
Soft tissue mobilization
Deep oscillation therapy
Microccurents therapy
These approaches can help stimulate blood flow, reduce inflammation, and promote tissue repair.
Improved circulation helps deliver nutrients to nerves while removing metabolic waste.
The Importance of Early Intervention
Diabetic neuropathy often progresses gradually, which makes early intervention critical.
When circulation problems are addressed early, it may be possible to:
Slow nerve damage
Improve nerve function
Reduce pain intensity
Prevent complications
Protect long-term mobility
Comprehensive metabolic testing, vascular assessments, and functional medicine evaluations can help identify underlying factors contributing to neuropathy.
Early detection allows for more targeted treatment strategies.
A Whole-Body Approach to Diabetic Nerve Pain
Diabetic neuropathy is rarely caused by a single factor. Instead, it often develops from a combination of:
Poor blood glucose regulation
Circulation problems
Inflammation
Nutritional deficiencies
Metabolic dysfunction
Addressing these root causes requires a whole-body approach that focuses on metabolic health, lymph and vascular circulation, and nervous system support.
Integrative strategies that combine medical care, lifestyle optimization, and therapeutic interventions often produce the most meaningful improvements.
Final Thoughts
Circulation plays a vital role in the development and progression of diabetic nerve pain. When blood flow becomes compromised, nerves receive less oxygen, fewer nutrients, and inadequate metabolic support. Over time, this lack of circulation contributes to nerve degeneration, inflammation, and chronic pain.
Understanding the relationship between circulation and neuropathy empowers individuals to take proactive steps to protect nerve health.
By improving blood glucose control, increasing movement, supporting vascular health, reducing inflammation, and enhancing circulation, it is possible to slow the progression of diabetic neuropathy and improve quality of life.
Early awareness and proactive care remain the most powerful tools in protecting the nerves from the damaging effects of diabetes.